User Guide - Billing Manager - Claims
Billing Manager Claims
In this section, we will discuss entering claim information into the Billing Manager.
IMPORTANT
Navigation within the Billing Manager application to move from one field to the next works best by hitting Tab on the keyboard. The application functions by providing additional information when Tab is used for navigating.
Claim General
Claim General tab is divided into the following sections:
· Patient and Providers
· Claim Payer Information
· Claim ID
· Relevant Dates.
The following is the Claim General screen:
Claim Payer Information
The fields in the Claim Payer Information are automatically populated based on the
details entered in the Patient and
Providers section. From Setup -> General -> Core Information if you check Use visit numbers and Use
additional A/C#s, you will be able to assign a claim with two additional
fields on Claim-General: the visit
number and the additional patient A/C#.
Relevant Dates
The claim forms are filled per the claim
form used by the insurance companies, some using the old form 1500 (08-05) and
some using the new 1500 (02-12).
·
1500 (02-12)-New Form
This is the new claim
form sent to the insurance companies. The information entered is recorded in
the patient details. The details required for the new claim form include:
·
1500 (08-05)-Old Form
This is the old claim
form sent to the insurance companies. The information entered is recorded in
the patient details. The details required for the old claim form include:
Claim Details
The following is the Claim Details screen:
Enter the necessary fields and click Save, and the line will automatically
change to number 2, allowing new claim details to be recorded. To modify existing
claim details, highlight the required line, make necessary changes and click Save as shown below.
The four main sub-sections under Claims Details are:
· ESPDT
· Anesthesia
· Dental
·
Facility Bill
Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) is a program which provides comprehensive and preventive health care services for children under the age of 21 who are enrolled in Medicaid. Select this feature only if the EPSDT details need to be entered on a claim.
The following are the additional fields required when EPSDT is selected:
Anesthesia
If the claim is an anesthesia claim, fill in
the diagnosis codes as before. After the
codes have been entered, check the box labelled Anesthesia. This will change
the service line information boxes to boxes for an anesthesia claim. The information is filled in the same way as
a regular claim. When complete, click Save. The information will be saved to
the grid as with regular claims. The following are the additional fields required
when Anesthesia is selected:
Dental
Select the box labelled Dental when a claim is for dental claim for a Community Health
Clinic. Currently we do not send Dental claims electronically to our
clearinghouse partners. The claims can only be printed. The
following are the additional fields required when Dental is selected:
After you have created a dental claim, you may print a standard ADA
claim form by clicking Print ADA Form on Claim-Final. The
printing form will open providing the same functionality as the CMS printing
form.
Facility Bill
Select the box labelled Facility Bill to display additional fields and to send a claim as an
837I electronic claim or on a UB-04 CMS-1450 form. To display the Facility
field you have to select a facility that has had the option selected from
Setup-Facilities. At this time we do not send every field for available
facility billing. Below is a list of the fields that are currently in the
product:
Claim-Final
Claim-Final tab is used to add any patient
co-payments received at the time of service, as well as any other authorization
codes that may be required.
The main sections on the Claim Final screen are:
· Patient Payment: The patient payment section is used for a patient that makes a co-payment. A co-payment can be entered in one of three ways:
1. Cash
2. Check
3. Credit/Debit Card
·
Other: used to enter additional
details regarding payment apart from the payment options mentioned above.
Patient Payment
Other

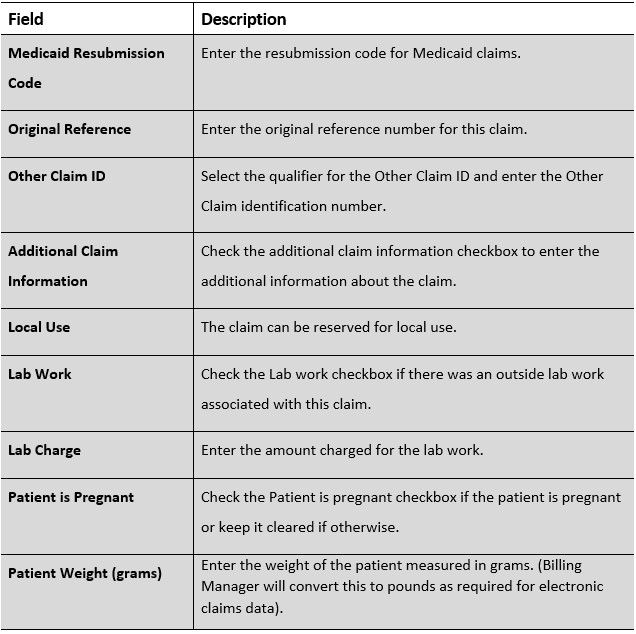
Attachment Details


Release
Release saves the claim and releases it per the debtor that need to be recorded. These recorded claims are saved in the required statuses and will reflect on the Today’s tab. Once a day these claims stored in their respective statuses are sent to our clearinghouse partner.
There are five ways to save a claim in Billing Manager:
1. Release as Voided: This option is displayed when an existing claim is loaded and only for practices with enabled Allow Sending Claims to EDI with a voided setting. This releases the claim with a Claim Frequency Code of 8.
2. Save as Pre-Released: This is used for claims that are incomplete or claims that have all the claim information, but may be missing the provider number for the payer.
3. Save for Review: This is used to place claims in the For Review bucket and is useful in situations when the user may be undergoing training. This allows those claims to be identified as requiring review prior to release.
4. Save for Client Review: Claims saved to this status can’t be released without moving the claim to another pre-released status first.
5.
Save for Billing Approval:
Claims saved to this status can be saved to any other pre-released status or
released to the clearinghouse.
Print Claims
The Print Claims screen on Claim-Final operates in two modes: by Patient and by Insurance Plan.
1. Patient Mode
The Patient mode allows the available filters to select individual claim copies for printing according to entered values. The list of claim copies displayed in the grid will be filtered automatically when any filter is changed. The following filters are available in the Patient mode:
· A/C#: Allows selecting patients to review their claims available for printing. The patient of the loaded claim will be selected automatically, if a claim was loaded on the Claim-General screen before the Print Claims screen is opened. Only claims of the currently selected patient will be displayed.
· Status: Allows reviewing only claim copies in a specific status. It will always list all available statuses, including those that do not allow printing. All Statuses option will be selected by default.
· Payer: Allows listing only claims released for a specific payer. It will list all payers available for the currently loaded patient, including the patient. All Payer’s option will be selected by default.
·
Claim: Lists individual unpaid claims of
the current patient, All Claims item allowing reviewing all claim copies for
all claims of the current patient, and Unpaid Claims option allowing reviewing
all claim copies of all unpaid claims of the current patient.
2. Insurance Plan Mode
The Insurance Plan mode allows bulk printing of all claims released for selected insurance payers. In the Insurance Plan mode, the available filters will not affect the number of displayed insurance plans to print claims (except for the Ins Type filter), but will only let claims matching the values selected in the filters to be printed instead.
The following filters are available in the by Insurance Plan mode:
· Type: Allows selecting only insurance plans of the specific type. The list of available plans will be filtered immediately when the selected Type is changed.
· Ins Payer: Allows printing only claims released for the insurance payers of the specific ranks. For example, only claims released for secondary payers will be printed if the Secondary item is selected in this filter. All payers option is selected by default.
· DOS From and DOS to: Allows printing only claims with DOS in the selected date range.
·
Status: Allows printing or previewing
only claim copies with a specific status. Please note that the filter contains
all active statuses, but not all of them allow printing. Only Preview will be
available for such statuses.
The Claim Form selection bar allows
selecting a claim form to print claims. UB-04 form will only be available if
the current practice has at least one facility with the Facility Billing option
enabled. ADA claim form will be available only if the current practice is a
Dental practice. Forms 1500 08-05, 1500 02-12, and IL DPA2360 forms will always
be available.
The Actions selection bar will allow actions such as printing or previewing the selected items, and reviewing and editing the printing settings.
In the Patient mode, printing and previewing
will only be available for claim copies which allow printing or previewing
according to the selected claim form. For example, it will not be possible to
preview claims on forms which do not have a preview yet (IL DPA2360 and ADA
claim forms); it will not be possible to print a standard claim on a UB-04
claim form (but printing of facility bill claims will be allowed on 1500 claim
forms).
The Omit Payments option will allow excluding the paid amount from the printed claim forms and previews. Amount Paid will not be displayed on previews and will not be printed when the option is checked.
The grid containing insurance plans (in the Insurance Plan mode) or claim copies (in
the Patient mode) allows selecting
several items simultaneously.
The Printing Settings button opens the Printing Settings screen. The following options can be modified:
- Currently selected printer
- Top and left margins are used to adjust position of the printout on the form.
- Font Size and Font Name are used to select a specific font to print the forms with and the size of the font. Values ranging from 5 to 14 are allowed for font size.
Also, test forms can be printed from the Printing Settings screen to test the selected settings.
Claims can now be previewed before printing to verify the claim data using the selected claim form. Preview is available from either Print Claims screen by selecting an item to preview, selecting the desired claim form, and selecting the Preview button.
Also, claims can be previewed from
- The Claim-General screen using the Claim History and Preview control;
To preview a claim copy from the Claim History and Preview control,
* load a claim on the Claim-General
screen,
* open the Claim History and Preview control,
* and either double-click the desired copy to open the Preview dialog,
* or use the context menu available on right-click on the desired claim copy.
Print Statement
This will print a current statement for the patient. You have the option to print a test statement or a full current statement. If you choose to select a Full Current Statement, you can either update the patient’s statement record or not. If you choose to update the patient’s statement record, a note will be made on that patient’s transaction history about the statement going out. This will also change the statement cycle.
Related Articles
Industrial Invoice Billing User Guide
Please find attached user guide under the Attachement tab.User Guide - Billing Applet - Patient Payments
User Guide for the Patient Payments module of the Billing appletUser Guide - Billing Applet - Setup
User Guide for setting up the Billing appletHow to print 1500 Claim Forms
Question How do you print out 1500 Claim Forms to send to the insurance carrier? Answer To print out a claim(s), first, you have to make sure you have clicked the Save Claim-Release button on all of the claims that you want to print. If claims are in ...Billing Applet 7.4 Release Notes
Please see attached release notes for new Billing Applet version 7.4.